Connect With Us

Foot and Ankle Trauma
Broken Feet
A broken foot can either refer to a fracture or a straight break. The location of any break can tell you how the break happened. Toes, for instance, break typically as a result of something being kicked hard and with great force. Heel breaks almost always are a result of an improper landing from a tall height. Twists or sprains are the other two frequent occurrences. As with all usual breaks, they result from unexpected accident or sudden injury. As with stress fractures, breaks form as a process over time from repeated stress on already present cracks. Runners, dancers, and gymnasts are the usual athletes who receive this type of break. Stress fractures result from incredible pressure on the feet. It is no surprise these athletes bear the majority of reported fractures.
Pain, swelling, bruising, and redness are all indicative of the typical symptoms from a broken foot. Severe pain—to the point of not being able to walk—usually depends on the location of the break in the foot. Toes are on the lower scale of pain threshold, but heels are high, as are a few other particular bones. As the severity of the broken foot increases, symptoms like blueness, numbness, misshaping of the foot, cuts, or deformities will become apparent. These symptoms indicate the need to see a medical professional with access to an x-ray facility.
Prior to seeing a specialist, precautions should be taken to reduce pain and swelling. Elevate and stabilize the foot, and refrain from moving it. Immobilization of the foot is the next priority, so creating a homemade splint is acceptable. Keep in mind that while creating a splint, any increase of pain or cutting off blood circulation means that the splint should be removed immediately. Use ice to decrease swelling and relieve pain symptoms.
When dealing with a medical center, the patient should note that the treatment can vary. The treatment will depend on the severity of the fracture and the cause of the break. Crutches, splits, or casts are common treatments while surgery has been known to be used in more severe cases in order to repair the break in the bones.
Broken Ankles
Broken ankles are a serious injury that can lead to an inability to walk, function, and also cause a significant amount of pain. A broken ankle is a break in one of the three bones in your body that connect at the ankle joint, the tibia, the fibula, and the talus. The tibia and fibula are your two primary leg bones that connect at the knee, which sits directly upon the talus bone. This is protected by a fibrous membrane that allows for movement in our ankle joint. A broken ankle is usually caused by the foot rolling under or twisting too far, causing one of these three bones to snap.
A broken ankle is different from an ankle sprain, which occurs when the ligaments are ripped or torn but no bones have been broken. A sprain can still be very severe, causing bruising in the foot and an inability to hold your own weight, much like a broken ankle would. If you’re unable to stand, and suspect that you have a broken ankle, the first thing to do would be to get an immediate x-ray to determine the severity of the break.
A common cause of broken ankles is when the ankle is rolled over with enough pressure to break the bones. This usually happens during exercise, sports, or other physical activities. Another common cause is a fall or jump from a tall height.
One immediate treatment for pain relief is elevating the feet above your head to reduce blood flow to the injured area. You can also apply ice packs to your ankles to help reduce swelling, redness, inflammation, and pain. After these initial steps, getting a cast and staying off your feet as much as possible will aid in the recovery of the broken ankle. The less movement and stress the ankle has to endure, the more complete it will heal. A doctor can determine if surgery is needed in order to heal correctly. In these cases, an operation may be the only option to ensure the ability to walk properly again, followed by physical therapy and rehabilitation.
It is highly important to determine if surgery is needed early on, because a broken ankle can become much more severe than you realize. If not professionally treated, the broken ankle will inhibit your walking, daily functioning, and produce a large amount of pain. Treating your broken ankle early on will help prevent further damage to it.
Flat Feet and Orthotics
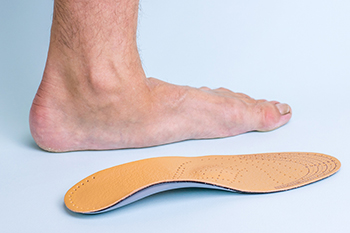
Flat feet, or pes planus, is a condition where the arches of the feet collapse, resulting in the entire sole of the foot being in contact with the ground. This can lead to various issues such as foot pain, arch strain, heel pain, and even knee, hip, and lower back problems due to altered biomechanics. Custom-made orthotics are often prescribed as a solution for flat feet. These orthotic devices are tailored to the individual's foot structure and biomechanics, providing support and alignment to address the underlying causes of flat feet. There are different types of orthotics available, including rigid orthotics that offer maximum support and control, semi-rigid orthotics that provide a balance between support and flexibility, and soft orthotics that offer cushioning and shock absorption. By correcting foot alignment and redistributing pressure, custom orthotics can alleviate symptoms associated with flat feet, improve foot function, and prevent or minimize the risk of further complications. If you have flat feet and they are interfering with your quality of life, it is suggested that you make an appointment with a podiatrist to see if orthotics can help provide correction and relief.
If you are having discomfort in your feet and would like to try orthotics, contact one of our podiatrists from Fox Valley Foot and Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Are Orthotics?
Orthotics are inserts you can place into your shoes to help with a variety of foot problems such as flat feet or foot pain. Orthotics provide relief and comfort for minor foot and heel pain but can’t correct serious biomechanical problems in your feet.
Over-the-Counter Inserts
Orthotics come in a wide variety of over-the-counter inserts that are used to treat foot pain, heel pain, and minor problems. For example, arch supports can be inserted into your shoes to help correct overarched or flat feet, while gel insoles are often used because they provide comfort and relief from foot and heel pain by alleviating pressure.
Prescription Orthotics
If over-the-counter inserts don’t work for you or if you have a more severe foot concern, it is possible to have your podiatrist prescribe custom orthotics. These high-quality inserts are designed to treat problems such as abnormal motion, plantar fasciitis, and severe forms of heel pain. They can even be used to help patients suffering from diabetes by treating foot ulcers and painful calluses and are usually molded to your feet individually, which allows them to provide full support and comfort.
If you are experiencing minor to severe foot or heel pain, it’s recommended to speak with your podiatrist about the possibilities of using orthotics. A podiatrist can determine which type of orthotic is right for you and allow you to take the first steps towards being pain-free.
If you have any questions please contact our office located in Naperville, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Foot Orthotics
Orthotics are shoe inserts that are meant to correct an irregular walking gait or provide cushioning to the feet. Orthotics come in a variety of different models and sizes, including over-the-counter and customizable variants. Customizable orthotics can be shaped and contoured to fit inside a specific shoe and are typically prescribed through a podiatrist who specializes in customized footwear and orthotics design and management.
Orthotics are beneficial because they can help prevent injuries from occurring and provide cushioning to keep pain levels down to a minimum. They also allow for the correct positioning of the feet. Orthotics can act as shock absorbers to help remove pressure from the foot and ankle. Therefore, orthotics can make bodily movements, such as walking and running, become more comfortable as well as help prevent the development of certain foot conditions.
Orthotics alleviate pain and make the foot more comfortable by slightly altering the angle at which the foot strikes the ground surface, therefore controlling the movement of the foot and ankle. Orthotics come in different variants and can be made of various materials. To determine what type of orthotic is most suited to your feet and your needs, it is best to consult your podiatrist. He or she will be able to recommend a type of orthotic that can help improve your foot function or prescribe a custom orthotic to best fit your feet.
Custom Orthotics For Foot and Heel Pain

Step into relief and reclaim your mobility! Foot and heel pain can be a thing of the past with the right Custom Orthotics. Customized to your unique foot structure, they provide the support and alignment needed to alleviate discomfort. Whether you're walking, running, or simply standing, Custom Orthotics ensure every step is cushioned and pain-free. Don't let foot ailments dictate your day. With Custom Orthotics, embrace a world of comfort and freedom. Call today to schedule an appointment.
What Is Tarsal Tunnel Syndrome?
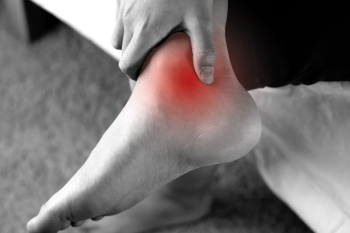 Tarsal tunnel syndrome is a compressive neuropathy condition that results from the entrapment of the posterior tibial nerve as it passes through the tarsal tunnel, a narrow passageway located on the inner side of the ankle. This entrapment leads to many symptoms, most notably pain, tingling, and burning in the foot and heel, which sometimes extends into the toes and lower leg. Many things can cause tarsal tunnel syndrome, such as injuries to the ankle, swelling from other health problems like diabetes, or just by repeating the same movements that irritate the area. Treatment strategies are tailored to the severity and underlying cause of the syndrome. Conservative measures include anti-inflammatory medications and orthotic devices to alleviate pressure on the nerve. More invasive options include surgical decompression to relieve the nerve entrapment. Tarsal tunnel syndrome can be hard to diagnose because its symptoms overlap with other nerve-related conditions. Podiatrists, or foot doctors, can do comprehensive evaluations to properly diagnose tarsal tunnel syndrome. If you have foot pain, or suspect tarsal tunnel syndrome, it is suggested that you seek treatment from a podiatrist who can properly diagnose this condition and offer a personalized treatment plan.
Tarsal tunnel syndrome is a compressive neuropathy condition that results from the entrapment of the posterior tibial nerve as it passes through the tarsal tunnel, a narrow passageway located on the inner side of the ankle. This entrapment leads to many symptoms, most notably pain, tingling, and burning in the foot and heel, which sometimes extends into the toes and lower leg. Many things can cause tarsal tunnel syndrome, such as injuries to the ankle, swelling from other health problems like diabetes, or just by repeating the same movements that irritate the area. Treatment strategies are tailored to the severity and underlying cause of the syndrome. Conservative measures include anti-inflammatory medications and orthotic devices to alleviate pressure on the nerve. More invasive options include surgical decompression to relieve the nerve entrapment. Tarsal tunnel syndrome can be hard to diagnose because its symptoms overlap with other nerve-related conditions. Podiatrists, or foot doctors, can do comprehensive evaluations to properly diagnose tarsal tunnel syndrome. If you have foot pain, or suspect tarsal tunnel syndrome, it is suggested that you seek treatment from a podiatrist who can properly diagnose this condition and offer a personalized treatment plan.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact one of our podiatrists of Fox Valley Foot and Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our office located in Naperville, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.
How Shoes and Orthotics Impact Walking

Wearing shoes can make it hard to study how your feet move while walking. But researchers found that if they looked at how the shin bone turns while walking, it relates to your heel's movement. Shoes and orthotics also affect shin bone rotation, both reducing how much the shin bone turns inside, compared to walking without them. Some special insoles slow down the shin bone movement, while hard insoles make the shin bone move more and faster. Patients can benefit from this research by making informed choices about the type of shoes they wear, as footwear plays a vital role in how the shin bone and heel interact during walking. Moreover, orthotic devices are commonly used to address various foot problems, and patients should be aware that the choice of orthotics can influence how their shin bone rotates while walking. Customized orthotic solutions, tailored to meet individual needs, can ensure optimal support and alignment. It is suggested that patients seek professional advice from a podiatrist to assess gait, foot mechanics, and specific requirements for shoes and orthotic devices, ultimately promoting better foot health and mobility.
The benefits of custom orthotics are far-reaching and can make a significant impact on your daily life. Whether you are an athlete looking to enhance your performance, a healthcare worker on your feet every day, someone who experiences chronic foot pain, or someone who wants to improve their overall comfort and well-being, custom orthotics can be a game changer.
Custom orthotics provide support, stability, and relief for a variety of foot conditions ranging from flat feet to heel pain. They can even help prevent injuries and address more severe foot concerns, such as plantar fasciitis and diabetic foot issues.
Contact one of our podiatrists at Fox Valley Foot and Ankle Specialists to create tailored orthotics for you and enjoy a higher quality of life, reduced pain, and increased mobility. With the right orthotics, you can continue doing the things you love, whether it’s running, dancing, or simply walking comfortably without discomfort.
If you are suffering from foot discomfort or have concerns about your foot health, do not hesitate to contact one of our podiatrists at Fox Valley Foot and Ankle Specialists to explore the benefits of orthotics for you. Your feet are the foundation of your body and investing in their well-being can lead to a happier, healthier, and more active lifestyle. Your feet will thank you!
If you have any questions please contact our office located in Naperville, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Investing in Custom Orthotics Means Investing in Foot Health
Custom orthotics offer a tailored approach to foot health, providing a host of benefits that extend far beyond conventional shoe inserts. One of the primary advantages lies in their ability to address specific biomechanical issues. Unlike off-the-shelf inserts, custom orthotics are crafted based on an individual's unique foot structure, gait, and any existing foot conditions.
The personalized design of custom orthotics ensures optimal support for the arches, promoting proper alignment and distributing pressure evenly across the feet. This can be particularly beneficial for individuals dealing with issues such as overpronation or underpronation, as custom orthotics help correct imbalances that may lead to discomfort or injury.
Beyond biomechanics, custom orthotics can alleviate a range of foot problems, including plantar fasciitis, bunions, and metatarsalgia. They provide targeted relief to areas under stress, reducing pain and inflammation. Additionally, for those with specific medical conditions like diabetes, custom orthotics can play a crucial role in preventing complications associated with poor foot health.
Comfort is another key aspect of custom orthotics. By accommodating the unique contours of an individual's feet, these inserts enhance overall comfort, making daily activities more enjoyable. Whether for athletes looking to optimize performance or individuals seeking relief from chronic foot pain, custom orthotics offer a versatile solution.
Investing in custom orthotics is an investment in long-term foot health. They not only provide immediate relief but also contribute to the prevention of future issues. With the ability to seamlessly integrate into various types of footwear, custom orthotics empower individuals to prioritize foot comfort without compromising on style. In essence, custom orthotics are a personalized prescription for happy, healthy, and pain-free feet.
How Podiatrists Treat Bunions
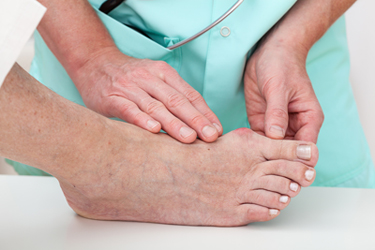 Podiatrists, or foot doctors, can take different approaches to treating bunions, which are structural deformities of the joint at the base of the big toe. This condition not only can cause pain but may also lead to a cascade of secondary foot problems, affecting mobility and quality of life. Initial treatment strategies may include non-invasive interventions aimed at alleviating symptoms and halting the progression of the deformity. Possible strategies include the use of custom orthotics designed to redistribute pressure away from the affected joint, targeted exercises to maintain joint mobility, and advice on appropriate footwear that accommodates the bunion without exacerbating discomfort. In more severe cases, podiatrists may recommend surgical intervention. This surgery, known as a bunionectomy, involves realigning the toe by correcting the abnormal angle of the bones, addressing the issue both cosmetically and functionally. If you have a bunion, it is suggested that you seek the care of a podiatrist who can recommend treatment options to prevent the condition from worsening.
Podiatrists, or foot doctors, can take different approaches to treating bunions, which are structural deformities of the joint at the base of the big toe. This condition not only can cause pain but may also lead to a cascade of secondary foot problems, affecting mobility and quality of life. Initial treatment strategies may include non-invasive interventions aimed at alleviating symptoms and halting the progression of the deformity. Possible strategies include the use of custom orthotics designed to redistribute pressure away from the affected joint, targeted exercises to maintain joint mobility, and advice on appropriate footwear that accommodates the bunion without exacerbating discomfort. In more severe cases, podiatrists may recommend surgical intervention. This surgery, known as a bunionectomy, involves realigning the toe by correcting the abnormal angle of the bones, addressing the issue both cosmetically and functionally. If you have a bunion, it is suggested that you seek the care of a podiatrist who can recommend treatment options to prevent the condition from worsening.
If you are suffering from bunion pain, contact one of our podiatrists of Fox Valley Foot and Ankle Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our office located in Naperville, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.